Meeting the health needs of the West Coast population is a complex business, further complicated by the challenges of delivering health services to a relatively small population over a large geographical area.
While many of the challenges we face are the same as other DHBs, our biggest challenge is our rurality.
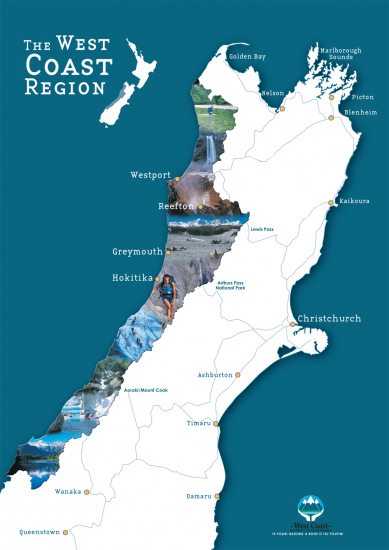
The total land area we cover is 23,283 square kilometres but our population is just 0.6% of New Zealand’s total population. Geographically we are the third largest DHB in the country but the most sparsely populated, with a population density of just 1.4 people per square kilometre.
Our geography creates significant challenges, often requiring patients or health professionals to travel long distances to receive or deliver services. This magnifies operating the pressures we face and means that we must consider all our other challenges with this overarching factor in mind.
Workforce challenges: Our workforce is relatively small, but must provide a broad range of complex services at a consistently high standard. In our rurally isolated environment we face significant difficulties in recruiting and retaining a suitable health workforce.
Facility pressures: A number of our current health facilities are outdated, inefficient and expensive to maintain. Many are poorly located and do not support the model of care needed to deliver our vision. Careful consideration must be given to the long-term future of all the facilities we own and operate.
Fiscal pressures: Meeting growing service demand, increasing treatment and infrastructure costs, and expectations around wages and salary increases is an ongoing challenge. We are also balancing community expectations regarding access to new and complex services in a small rural environment.
In meeting these challenges the West Coast will become a leader in the provision of rural health services: identifying opportunities to add value, reducing duplication across our system, and redirecting funding into services that will provide the greatest return in terms of health gain.
We have taken important steps towards enabling our vision, including connecting clinical information systems, establishing shared transalpine pathways with the Canterbury DHB, introducing the Complex Clinical Care Network and commencing the development of Integrated Family Health Services.
We have been deliberately investing in a rural generalist model, a proven strategy for creating a more integrated and sustainable workforce in more remote rural health systems. It involves all professions – medical, nursing, midwifery and allied health – working to the full extent of their scope of practice as members of a multi-disciplinary team. A rural generalist doctor, for example, may be qualified to work in both general practice and hospital settings with a speciality in obstetrics or anaesthetics. They would also be supported by local and Christchurch-based specialists, enhancing the capacity, capability and resilience of our health system.
Developing a core workforce of rural generalists will improve the sustainability of services, support a more integrated model of care and provide continuity of care for our population. By improving service access, it will also help us to support people to stay well, reduce health inequities and improve health outcomes – all key goals for our health system.
As part of the expansion of their scope of key clinical roles, professionals can access education and leadership training.
The West Coast DHB will always need to refer people to larger centres for highly specialised care, such as: neurosurgery, forensic services, some cardiac care and cancer treatments, specialised burns treatments and neo-natal intensive care.
The following critical success factors are the strategic components needed for us to achieve our vision and become a leader in the provision of rural health services.
The integration of services to improve patient flow: